 
The QTc is prolonged in patients with congenital long QT syndrome (CLQTS). The corrected QT interval is known as QTc, and it is prolongation of the QTc, rather than the QT, that determines the risk of TDP. Thus, there is a requirement to “correct” the QT interval, particularly in hospital settings where the resting heart rates of patients may not be normal. During tachycardia, the QT interval decreases, and in bradycardia, it lengthens. We present an approach to the ECG in this context, and a step-by-step guide to manually measuring and correcting the QT interval, and an approach to management in common hospital-based clinical scenarios.Īdditionally, the normal limit for the QT interval varies with heart rate. A wealth of correctional formulae have been derived, but none has proven superior. Therefore, the QT interval often requires “correction” for the current heart rate, in order to correctly stratify the risk of torsades de pointes. This is a difficult task, as the normal QT interval is typically measured relative to the heart rate. Automated ECG printouts cannot be relied upon to diagnose QT interval prolongation thus, the onus is on the clinician to identify it. Detection of a prolonged QT interval is essential as this can be a reversible problem, particularly in the context of the use of a variety of commonly prescribed medications in the hospital setting. Abnormal prolongation of the QT interval can lead to torsades de pointes, a form of potentially life-threatening polymorphic ventricular tachycardia (VT). 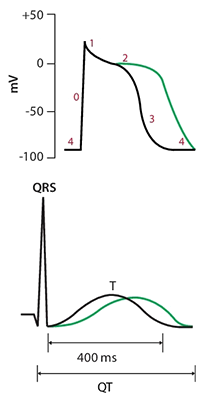
This interval represents the time taken for the ventricles to completely repolarise after activation. One of the more challenging aspects of ECG interpretation is measurement and interpretation of the QT interval. 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
